Detection
Understanding How Clinicians Categorize Scoliosis
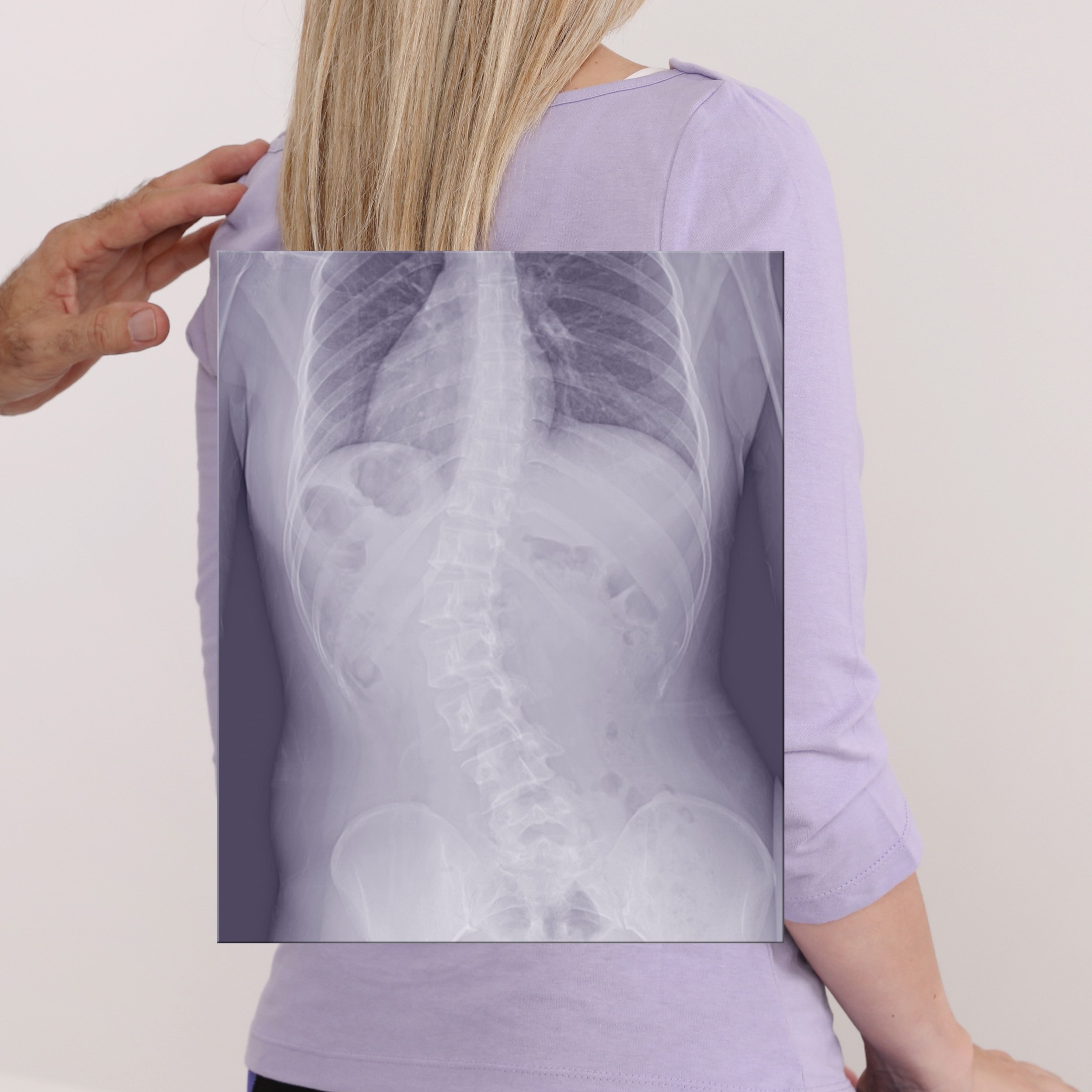
Scoliosis is a three-dimensional condition of the spine. When viewed from the back (coronal plane), the spine may appear as a "C" or "S" shape, instead of an “I” shape. However, it is rarely just a side-to-side curve; in almost all structural cases, the vertebrae also rotate in the axial plane (the view from above), similar to the twist of a corkscrew. This rotation often causes the back to lose its natural curves when viewed from the side (sagittal plane) and appear flatter. Together, these 3D changes can lead to visible shifts in symmetry, such as a rib hump or an uneven waistline. Specialists typically categorize scoliosis into different types:
- Idiopathic Scoliosis: The most common category (approx. 80%), where the exact cause is still a mystery. Doctors break this down by age: Infantile (birth to 3), Juvenile (ages 3 to 10), and the most frequent type, Adolescent Idiopathic Scoliosis (AIS), which typically shows up during the major growth spurts between ages 10 and 18.
- Congenital & Neuromuscular: Clinicians identify congenital cases as those involving vertebrae that did not form correctly during development. Neuromuscular cases are associated with conditions that affect the nerves or muscles supporting the spine.
- Structural vs. Functional: A structural curve is considered part of the spine's physical shape. A functional curve is often a temporary appearance of a curve caused by external factors like a leg-length difference.
- Syndromic Scoliosis: Develops as a result of an underlying syndrome, such as Marfan syndrome or Neurofibromatosis.
- Traumatic or Pathological: Rare cases where the curve is triggered by a specific injury, spinal infection, or tumor.
- Degenerative Scoliosis: Caused by the gradual breakdown of spinal discs and joints later in life.
Clinical Terms & Regions
Clinicians use specific terms to describe the location and direction of a curve:
- Thoracic: The mid-back region (T1–T12). Because these vertebrae attach to the ribs, rotation here may cause a visible "rib hump."
- Lumbar: The lower back (L1–L5). These are the largest vertebrae that bear the most body weight.
- Thoracolumbar: A curve with an apex (the peak of the curve) at the junction of the thoracic and lumbar spine.
- Cervical: The neck (C1–C7).
- Dextroscoliosis vs. Levoscoliosis: These terms describe curves that bow to the right side of the body (Dextro) or the left (Levo). Thoracic curves are most commonly Dextro; a Levo thoracic curve is less common and frequently warrants additional evaluation to rule out underlying factors.
Clinical Assessment & Screening
A thorough evaluation involves several tools and checks to help healthcare professionals understand both the shape of the spine and the health of the nervous system:
- Cobb Angle: A universal measurement taken from an X-ray or MRI to quantify the degree of curvature. Clinicians typically use 10 degrees as a diagnostic threshold.
- Scoliometer & Adam’s Test: These standard screening tools are used during physical exams to measure the Angle of Trunk Rotation (ATR). By having the patient bend forward into flexion, the 3D twist of the spine and related asymmetries—such as a rib hump—become more visible, helping to identify structural curves that may require further diagnostic imaging.
- Neurological Screening: Specialists perform routine checks of reflexes, muscle strength, and balance to rule out spinal cord involvement. This may include "superficial abdominal reflexes" or tandem gait testing to assess central nervous system health.
- Specialized Nerve Root & Tension Tests: While AIS is usually painless, providers may perform a Straight Leg Raise (SLR) to ensure nerves are moving freely. In specialized clinics, they may also utilize the Slump Test or Modified Cox Leg Raise to evaluate spinal cord tension and nerve sensitivity that may be associated with the curve.
- Skeletal Maturity: Tools like the Risser Sign or Sanders Scale use imaging to estimate how much growth remains, which helps predict the risk of curve progression.
Common Visual Indicators
Scoliosis is often first identified through subtle changes in physical symmetry, particularly during rapid growth spurts. Common indicators observed during clinical screenings include:
- Shoulder Alignment: Uneven shoulder height or one prominent shoulder blade.
- Waist & Hips: An uneven waistline or hips that appear shifted to one side.
- Clothing Fit: Asymmetry in how clothing hangs (e.g., uneven hemlines).
- Forward Bend: A visible "hump" or unevenness on one side of the back when leaning forward.
- Head Position: Head isn’t centered over the body.
Screening for Underlying Drivers
In some cases, a spinal curve is a symptom of an underlying condition rather than a standalone issue. Specialists perform comprehensive screenings—often utilizing advanced imaging like MRIs or genetic consultations—to rule out "hidden drivers" within the spinal canal or broader system. While these findings are only present in a small percentage of cases, this level of rigor ensures no stone is left unturned. Specialists investigate several categories, including:
- Neurological Indicators: During a clinical evaluation, a doctor looks for signs of internal factors such as a Syrinx (a fluid-filled cyst), a Tethered Cord, or a Chiari Malformation.
- Syndromic & Connective Tissue Factors: Screening may include looking for signs of conditions like Marfan Syndrome, Ehlers-Danlos (EDS), or Loeys-Dietz. These often require a multi-disciplinary approach to care.
- Other Clinical Indicators: Because every child is unique, specialists also monitor for subtle neuromuscular or metabolic indicators that might influence how a curve progresses or how it should be managed.
The Importance of Family History
Scoliosis and many of its related conditions can have a genetic component. When meeting with a specialist, it can be helpful to share if any family members have experienced:
- Spinal Conditions: A history of scoliosis, kyphosis, or early-onset back issues.
- Connective Tissue Traits: Family members who are exceptionally tall with long limbs or experience extreme joint hypermobility (double-jointedness).
- Neurological or Cardiac History: Any history of heart valve issues or spinal cord conditions.
You Are Not Alone
Finding out your child has scoliosis can feel overwhelming. Remember that with modern intervention, the vast majority of children with scoliosis go on to live active, healthy, and normal lives.
Considerations for Your Journey
Finding the right path forward is a process. Many families find it helpful to:
- Organize Records: Maintain a folder of imaging reports and growth measurements to bring to every appointment.
- Gather Questions: Prepare a list of questions for a specialist. Since specialists are often located in larger cities, many families plan for travel to access specific expertise or second opinions.
- Discuss Imaging Technology: Many modern scoliosis clinics utilize or refer to low-dose radiation (such as EOS) or no-radiation (standing MRI) imaging options. Because scoliosis often requires frequent monitoring during growth, you may wish to ask your healthcare provider which imaging method is most appropriate for your child’s specific needs and long-term health.
References: SRS–Lenke–Aubin 3D Classification: Aubin, C. E., et al. "The SRS–Lenke–Aubin 3D classification of adolescent idiopathic scoliosis," Spine Deformity Journal (2026). AIS Overview: "Adolescent Idiopathic Scoliosis: Comprehensive Pathoanatomy," Nature Reviews Disease Primers (2025). Clinical Guidelines: "Assessment and Management of AIS," Paediatrics & Child Health (2025). Patient Education: "Scoliosis Patient Resources," American Association of Neurological Surgeons (AANS) (2024).